Background:
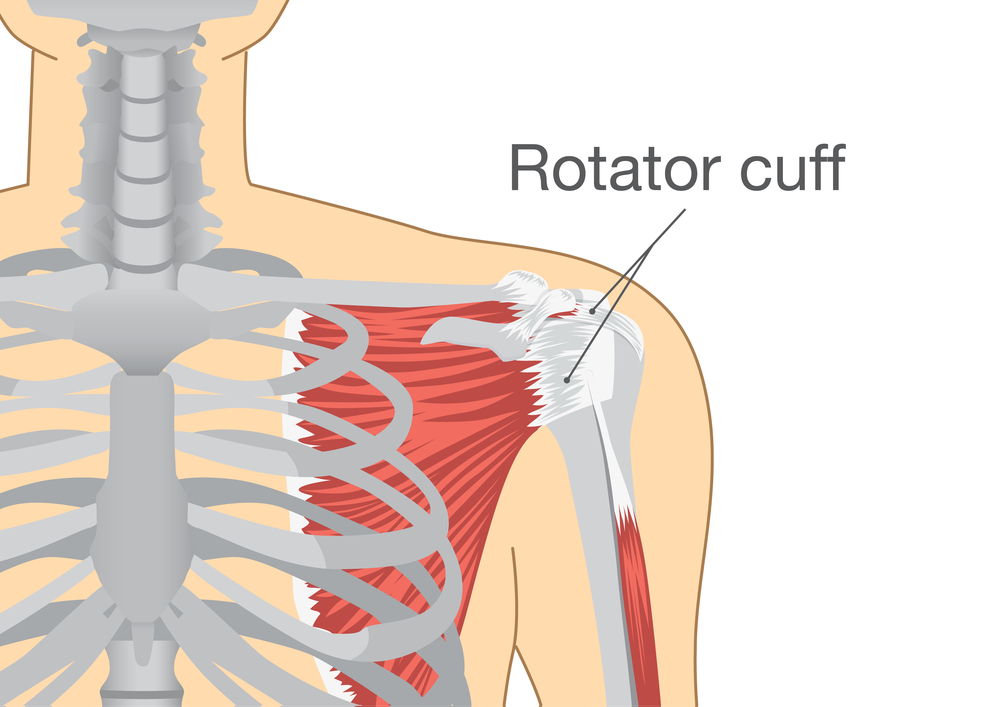
The use of platelet-rich plasma (PRP) for the treatment of rotator cuff disease is still controversial. The purpose of the present study was to investigate the safety and efficacy of a fully characterized allogeneic pure PRP injection into the subacromial space of patients with rotator cuff disease in comparison with corticosteroid injection.
Methods:
A 2-group, parallel, assessor-blinded, randomized controlled trial was conducted. A total of 60 patients with clinically and structurally diagnosed rotator cuff disease were randomly assigned to receive a subacromial injection of either 4 mL of allogeneic pure PRP or a 4-mL mixture of 1 mL of 40-mg/mL triamcinolone acetonide and 3 mL of 2% lidocaine under ultrasonographic guidance. The primary outcomes were safety and the Constant score at 1 month. The secondary outcomes were pain, range of motion, muscle strength, functional scores, and overall satisfaction and function.
Results:
There were no treatment-related adverse events. The Constant score at 1 month did not significantly differ between the PRP and corticosteroid groups. At 6 months, the DASH (Disabilities of the Arm, Shoulder and Hand) score, overall function, and external rotation were significantly better in the PRP group than in the corticosteroid group, and the other clinical outcomes did not show significant differences. All pain measurements, the strength of the supraspinatus and infraspinatus, and 5 functional scores also improved slowly and steadily after injection, becoming significantly better at 6 months compared with those before the injection, whereas those in the corticosteroid group responded promptly but did not further improve.
Conclusions:
Allogeneic PRP injections for the treatment of rotator cuff disease are safe but are not definitely superior to corticosteroid injections with respect to pain relief and functional improvement during 6 months. The DASH score, overall function, and external rotation were significantly better in the PRP group than in the steroid group at 6 months. Generally, PRP slowly but steadily reduced pain and improved function of the shoulder until 6 months, whereas corticosteroid did not.
Level of Evidence:
Therapeutic Level I. See Instructions for Authors for a complete description of levels of evidence.
Copyright © 2020 by The Journal of Bone and Joint Surgery, Incorporated




 346-220-8063
346-220-8063